There are a lot of people who are asking this question, and the answer is yes – it is possible to use residential proxy networks without getting caught.
Can a proxy really hide your identity
There are a lot of concerns about online privacy and security. Many people worry that […]
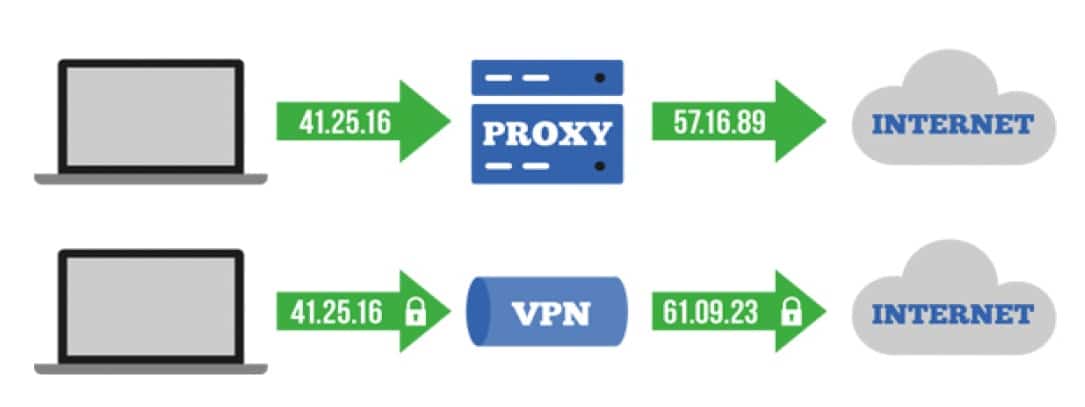
What’s better – proxy or VPN
So you’re trying to decide whether to use a proxy or VPN service to secure […]
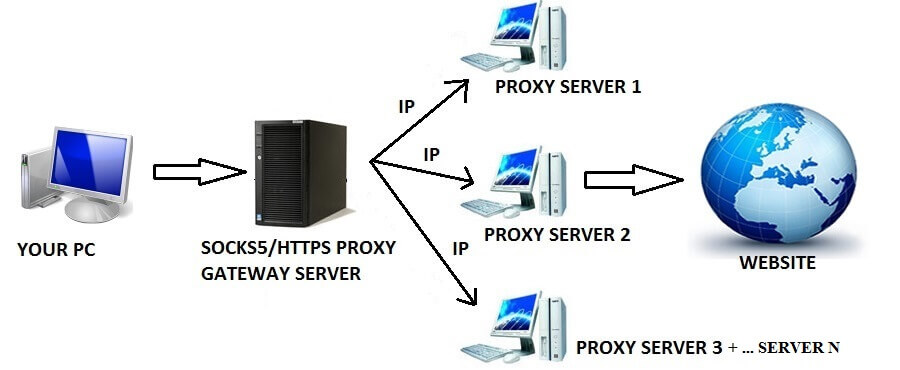
How proxy rotating companies have residential ip
If you’re looking for a comprehensive guide on how to find the best proxy rotation […]
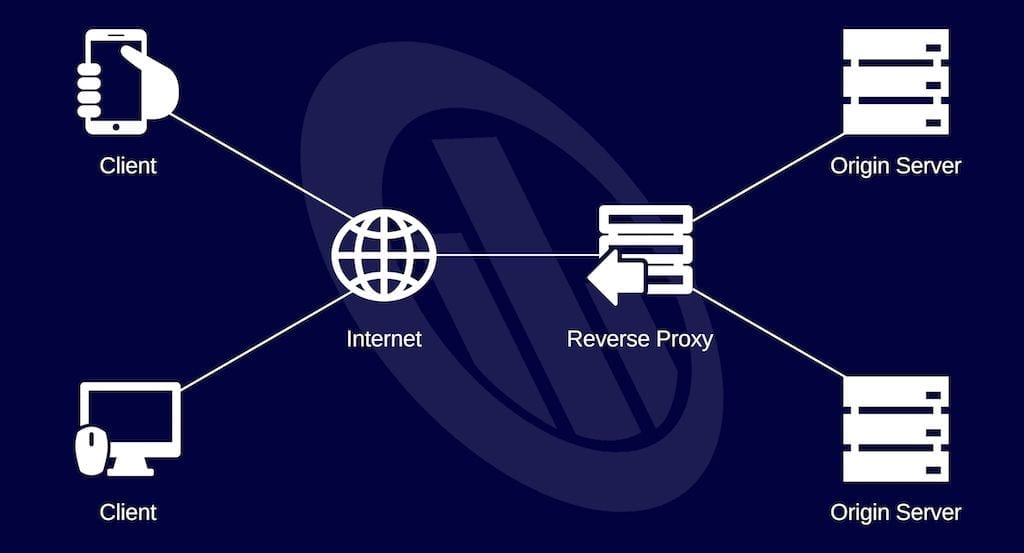
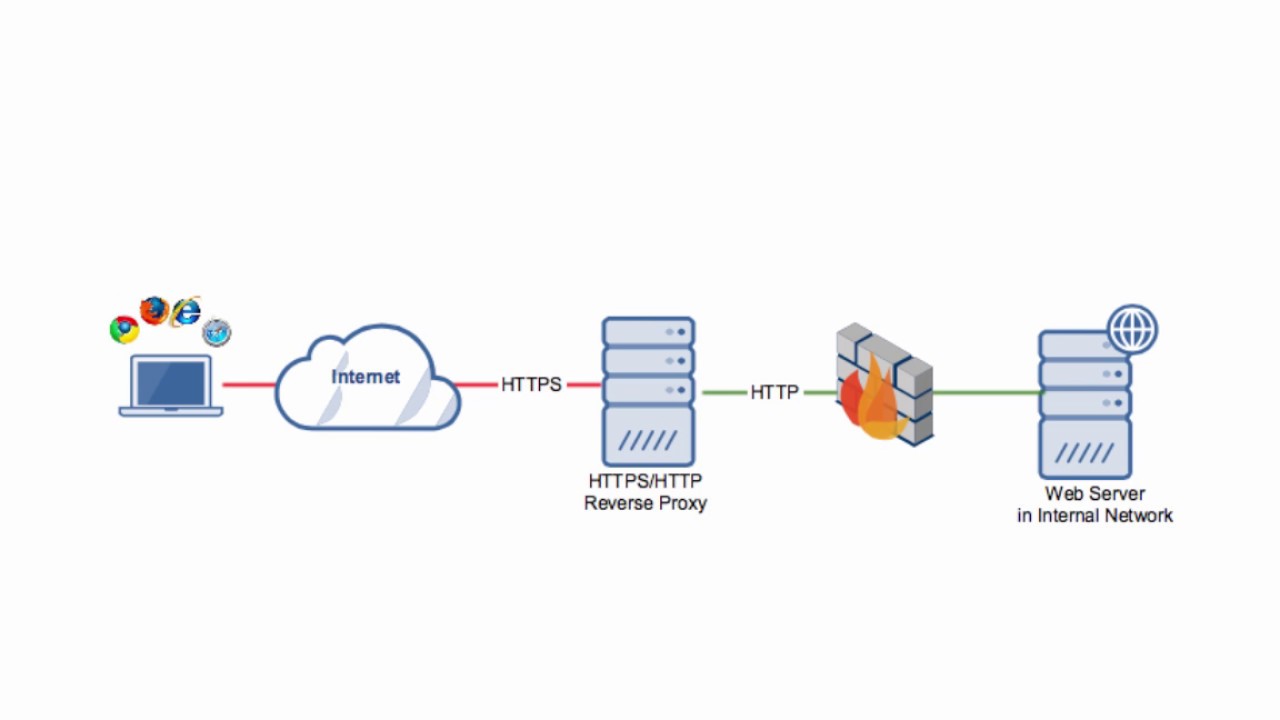
Why use a proxy server at home
A proxy server at home can provide a layer of security for your online browsing […]